Police Officer Suicide and Suicide Prevention
Tony Ford
It is a sad fact that police officers are more likely to die from suicide than in the line of duty. In 2020, 116 police officers died by suicide while 113 died in the line of duty (Stanton, 2022). In 2021, that number rose to 150 officers dying by suicide (Leone, 2022). Tragically, law enforcement officers have a 54% increase in suicide risk when compared to the civilian population (McAward, 2022). The problem seems to be even worse in smaller departments, which may not have an extensive support system or peer support resources. A 2012 study published in the International Journal of Emergency Mental Health found that departments with less than 50 full-time officers had a suicide rate over triple that of departments that had over 500 full-time officers (Volanti, et.al, 2012). This is concerning, as 49% of the police departments in the United States employ less than 10 full-time officers (Volanti, et.al, 2012).
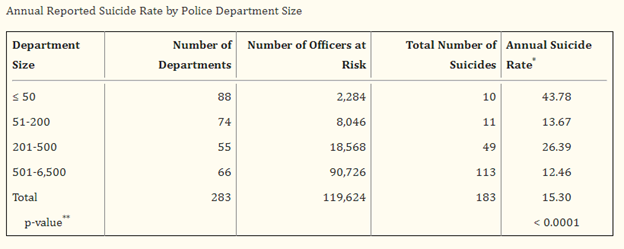
Figure 1 Courtesy of the National Library of Medicine. Figures are per 1,000 officers.
In the United States, most suicide attempts among the general population are not fatal (McAward, 2022). Yet, when a firearm is used, the chances of a suicide attempt becoming fatal skyrocket. Suicides that involve a firearm have a fatality rate greater than 82% (McAward, 2022). Police officers nearly always have a firearm available. In fact, the majority of law enforcement suicides happen at home, using the officer’s own service weapon (McAward, 2022).
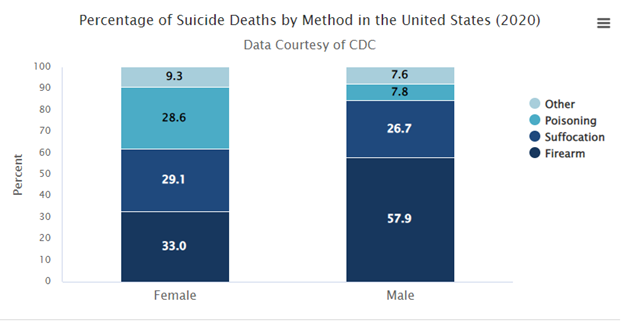
Figure 2 Data courtesy of the CDC
Though more study is needed, the lower suicide rate in larger departments may indicate that many of the mental health and peer support programs in use are having a beneficial effect. My department, which is over 500 sworn officers, has a robust peer support system that has officer volunteers. These volunteers go out to officer-involved shootings to offer support for officers that may need them. In addition, in 2021 we hired an on-staff clinician. She also comes out to deadly-force incidents and is available to speak with the officers. No officer is forced to take advantage of either resource, but they are there if needed. The peer support system has become more robust over time, with more and more offices volunteering to serve in the program. The clinician is also available for counseling services, and officers may go for a session either on or off duty. They do not have to involve their chain of command in the scheduling, and the clinician provides nothing other than a work excuse note. The clinician will also likely become more effective as she spends time with officers and learns the stressors of the job. The support is welcome, as we have lost three officers to suicide since I started in 2002.
There are other things departments can do for suicide prevention. John Becker, a former police officer turned clinician in Pennsylvania, recommends programs for positive stress relief, such as softball, basketball, or bowling leagues (Becker, 2016). He also says that supervisors have a role to play in ensuring open communication (Becker, 2016). Support, he says, doesn’t have to be a group hug. Simply asking a subordinate how their shift went that day would encourage communication (Becker, 2016). He also points out the numerous benefits of better mental well-being in a police force, benefits that extend beyond suicide prevention (Becker, 2016). A healthy department will have fewer complaints and lawsuits, fewer officers calling in sick, fewer grievances and resignations, and even fewer on-the-job injuries (Becker, 2016).
There is no field quite like policing. The higher occurrence of suicides in the field should be met with programs and professionals who understand what officers are going through. Many times the best professionals for that task are other police officers. Departments should strive to have a holistic approach to officers’ mental well-being, and show officers that they care about their mental health. A department that ignores this important aspect of employee care is doing a disservice to their officers and the public that they serve.