Tagged: blindness
The Numbers are All in Your Head
Numbers. Those arithmetical values that allow us to analyze and measure our surroundings. Without them, our understanding of the world we live in would be far less interesting. But what may be even more interesting is the way we process those numbers and how closely related that process is to spatial reasoning. The connection between space and numbers, specifically how we materialize values in our heads through mental number lines has been studied over the years, revealing that spatial orientation is incredibly important to this hypothetical number line. One study led by cognitive neuroscientist Stanislas Dehaene investigated how number magnitude is spatially organized in our minds and introduced the phenomenon of Spatial-Numerical Association of Response Codes, or the SNARC effect for short.
More
Visual Deprivation Could Improve Hearing in Adults
 Most people are familiar with the idea that people who are blind have better hearing than those with normal vision. It was formerly thought that this compensation for lack of vision could only develop in the brains of the very young. However, new research conducted at the University of Maryland and Johns Hopkins University suggests that the brain may be more flexible than previously believed.
Most people are familiar with the idea that people who are blind have better hearing than those with normal vision. It was formerly thought that this compensation for lack of vision could only develop in the brains of the very young. However, new research conducted at the University of Maryland and Johns Hopkins University suggests that the brain may be more flexible than previously believed.
In the study, researchers kept one group of healthy mice in total darkness for a week, and exposed the other group to natural light for a week. Then the team used electrodes to measure activity in neurons in the mice’s primary auditory cortex. This is the part of the brain that processes how loud a sound is and its source. By analyzing this data, researchers found that the mice who were exposed to a week of darkness had much better hearing than the control mice.
This suggests that the circuits that process sensory information can be re-wired in the brains of adult mice, even after the early critical period for hearing. These findings seem to contradict the idea that once the critical period for hearing is past, the auditory system doesn't respond to changes in an individual's soundscape.
Engineering the Blind to See
Vision is one of the most impressive functions of the human brain. It interprets nothing but electromagnetic waves and paints a glorious picture of our daily existence from the scattered chaotic sea of intertwining light waves that we call home. Many see their vision deteriorate and the world blur as time goes on and these problems can be corrected by optometry, but blindness comes on like a relentless infidel for more than two million people worldwide in the form of retinitis pigmentosa (RP). RP is a heritible genetic disorder that leads to degeneration and loss of function in the retina's photoreceptor cells, and can lead to full blindness in a matter of years. There is no cure or treatment for RP, but new research may change that very soon.
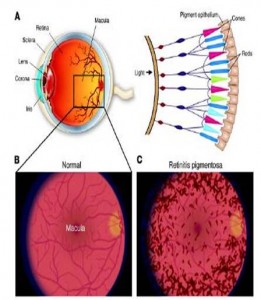
TOP: Macroscopic human eye (left) and rod and cone cell arrangement on the retina (right). BOTTOM: Normal human retina (left) and human retina with retinitis pigmentosa (right)/(Source: Medical-Look.com)
Vision starts in the photoreceptor when light activates rhodopsin, a G-protein coupled receptor pigment consisting of light sensitive opsin and retinal. Light triggers a conformational change in retinal that kick starts a G-coupled visual cascade and the flow of visual information to the brain. In retinitis pigmentosa, rhodopsins in the photoreceptors become insensitive to light starting in the rod cells, and blindness sets in gradually. Rod cells are used in low light and deteriorate first, leading to night blindness, and dysfunction in cone cells used for color vision and acuity sets in until full blindness plagues the individual. Fortunately, a team of French scientists has investigated this degradation and has found a way to combat it by reactivating the photoreceptor cells through genetics. Their study was featured in the July 23rd issue of Science.
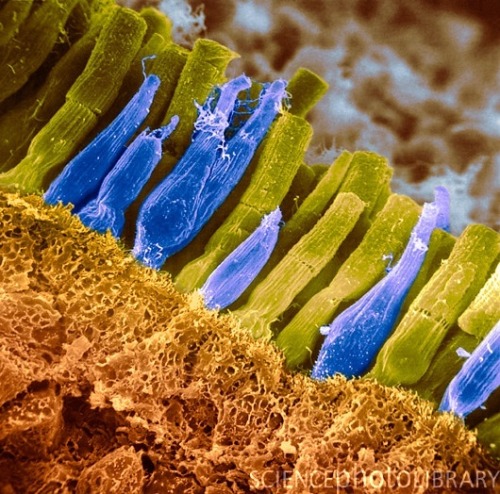
Artificially colored micrograph image of retinal rods (yellow-green) and cones (blue). (Credit: Science Photo Library @ sciencephoto.com)
The scientists isolated an achaebacterial rhodopsin analog called halorhodopsin that functions in the yellow and green wavelength range. They then introduced a halorhodopsin encoding gene into retinitis pigmentosa model mice via a viral vector and also created a control group. In their experiments, it was found that both slow and fast degrading retinal cells in the experimental mice regained their light sensitivity in response to integration of halorhodopsin into their insensitive photoreceptor cells. Electrical responses were recorded from ganglion cells (the third tier cell in the visual cascade) and healthy photoreceptor spikes were observed in response to light stimulation. Most importantly, lateral inhibition (the mechanism by which the brain discriminates edges of objects) was fully preserved, while mono-directional movement was retained. Halorhodopsin mice also performed significantly better than the control RP mice in a battery of visually guided tasks, demonstrating that their photoreceptors had been successfully resensitized by halorhodopsin integration. The scientists also tested the resensitizing ability of halorhodopsin on cultured human retinal cells. They were successful in integrating halorhodopsin into human cells via viral vectors, but could not conduct any clinical trials. However, photoreceptors expressing halorhodopsin demonstrated photocurrents and photovoltages that would be adequate to restore human vision.

Theoretical device that allows a halorhodopsin treated patient to see by projecting patterned light onto the eyes derived from camera input. (Credit: Y. Greenman/Science)
This opens the door to treatment of retinitis pigmentosa in the genes - the same place where it starts. Although halorhodopsin therapy will not fully restore all wavelengths in human vision, it can still serve as a tool to bring restore vision in the blind through optical devices. For example, an RP patient could be treated with halorhodopsin gene thearpy, then outfitted with a device that images the visual field and translates it into halorhodopsin recognizable wavelengths. This light mosaic is then projected onto the patient's eyes and the can "see" what is in front of them. The supplied image of the device is from a perspective article in the beginning of the current issue of Science.
View the full text Science article here (HTML) or here (PDF) and the perspective piece about the article here. Be sure to discuss in the comments!
Sources:
Seeing the Light of Day - Science (Perspective)
Genetic Reactivation of Cone Photoreceptors Restores Responses in Retinitis Pigmentosa - Science (Research Article)